Man given 5 percent chance to live survives thanks to Idaho’s only burn center
Published at | Updated at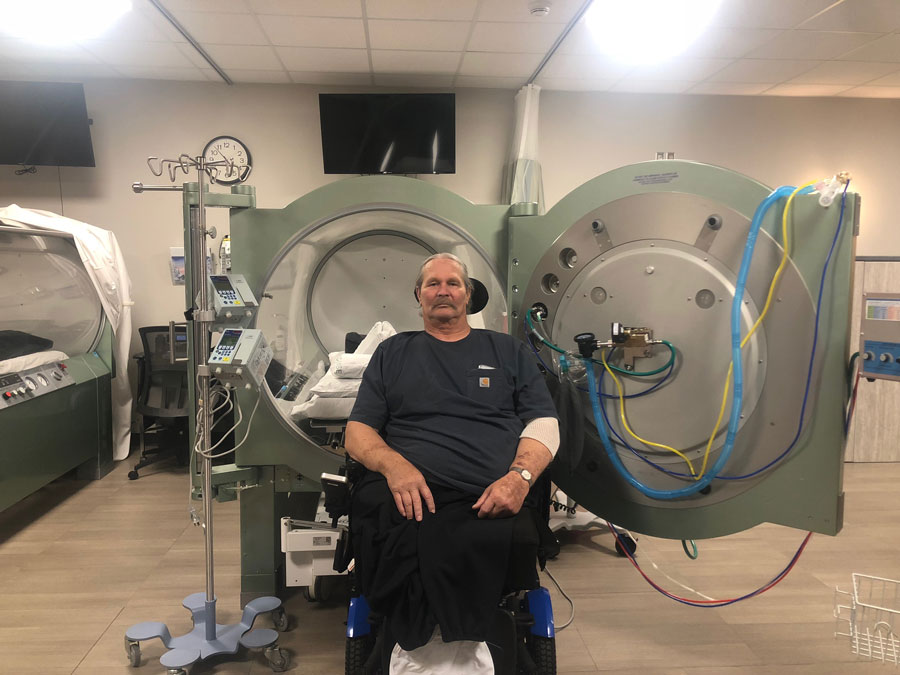
IDAHO FALLS — When Kris Heald went to his doctor thinking he had a urinary tract infection, he had no idea Eastern Idaho Regional Medical Center’s burn unit would end up saving his life.
For about two weeks, the 61-year-old, who was living in Salmon, felt like something wasn’t right with his body. He visited with his doctor about it, but things kept getting worse.
Eventually, he went to the local emergency room on April 14 for what he thought would be treatment for a UTI or bladder infection. Instead doctors told him he needed to be airlifted to EIRMC. He was diagnosed with necrotizing fasciitis, a rapid flesh-eating bacteria, and was given a 5 percent chance of survival.
“When I got on the plane, and we left the Salmon airport, that’s the last I remember until three weeks later,” Heald says.
Thirteen days before he was admitted to EIRMC, the hospital opened the first burn care center in Idaho, and with it, the only place in Idaho that could give him the treatment he needed.
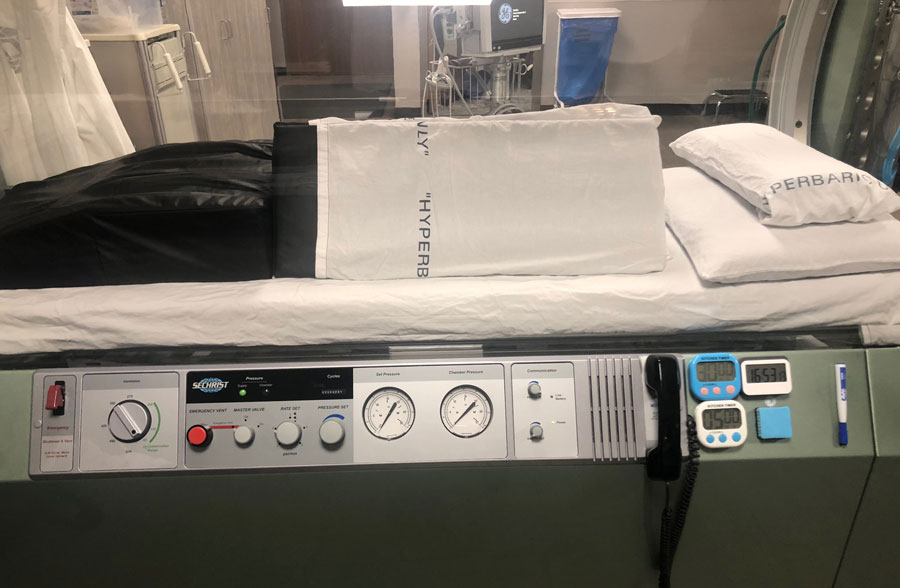
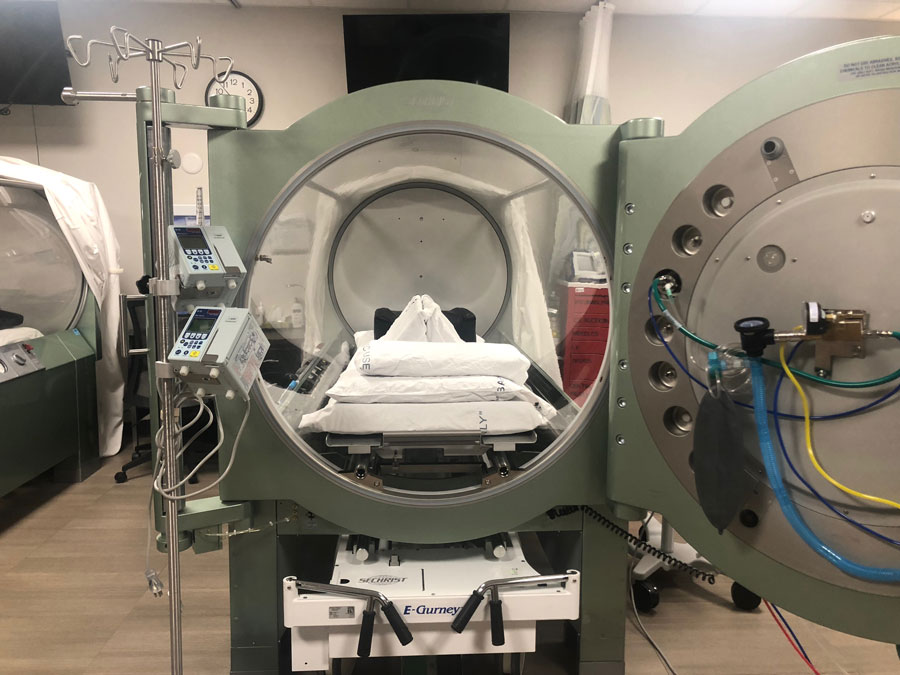
Heald was put on a ventilator and needed hyperbaric oxygen therapy, a treatment that allows patients to breathe pure oxygen inside a sealed container to accelerate the healing process.
“They basically oxygenate the environment like you were (scuba) diving, and then they have to bring you back up to regular oxygen surface just like you do when you dive,” EIRMC spokeswoman Coleen Niemann says.
Hyperbaric oxygen therapy is used to treat conditions such as non-healing diabetic wounds, bone infections, carbon monoxide poisoning and people with skin graphs or skin flaps.
EIRMC has had hyperbaric oxygen therapy for years, but before the hospital opened its burn center, it didn’t have the capability to treat critical care patients like Heald, who had to be on a ventilator during the process.
“If you’re on a ventilator because you’re critically injured or ill, you have to have very specialized equipment and specialized nurses to put a person who’s on a ventilator in a hyperbaric chamber,” Niemann says. “We’re the only place in the state of Idaho that does that.”
Heald was the first critical care patient in the EIRMC burn program.
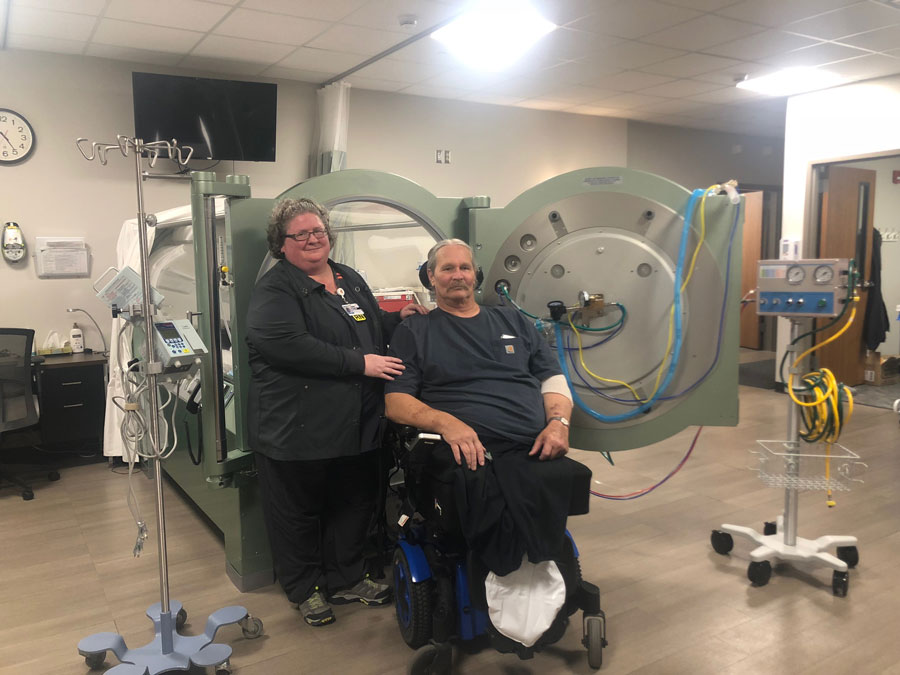
Michelle Fullmer, the lead hyperbaric technologist and a registered nurse, says Heald’s infection was similar to how one would treat a burn because of the tissue, fluid and volume loss.
For three days, he was on medications while in the ICU that made it so he couldn’t go in the chamber. But on April 17, he began his first of 10 critical care treatments (where he was ventilated and intubated) and first of 55 overall sessions in the chamber. To treat his infection, he needed to spend a little over two hours in the tube for each session.
“I’m overly thankful that I’m still alive,” Heald says.
Getting to the point where EIRMC could put patients on ventilators in a chamber didn’t happen overnight. The hospital partnered with the nation’s largest provider of inpatient burn care the Burn and Reconstructive Centers of America, who takes care of 20 percent of all inpatient burn victims in the country.
“All of our training, infrastructure, the technology we needed, the upgrades we needed, the people, the equipment, that was all part of a partnership that gave us that expertise,” Niemann says.
Fullmer mentioned that EIRMC is also the only facility in the region and state that treats critical care pediatric patients in their own facility. As far as she’s aware, the LDS Hospital is the only institution in Utah that does ventilator capable hyperbaric oxygen therapy for adults and pediatrics.
Since Heald’s case, more patients with necrotizing fasciitis have been seen at EIRMC. Fullmer said burn trauma doctors explained to her why there seemed to be a sudden increase in patients with the infection.
“They said, ‘They’ve always been sent to Utah because we couldn’t handle that level of severity,” Fullmer was told. “Now, we’re able to do this for the community and keep them here and closer to home.”
Heald has since moved to Idaho Falls to be closer to the hospital for ongoing treatment.