Concerning or overhyped? Can you compare COVID to the flu?
Published at | Updated at
IDAHO FALLS — Is the global COVID-19 pandemic really just a flu bug that’s getting more attention than it deserves?
That’s a question on the minds of more than a few people in eastern Idaho.
With influenza season beginning and COVID-19 cases continuing to surge, odds are you’ve heard people express this opinion. Some people think COVID-19 should be downplayed because of its similarities to the flu. Influenza affects countless people every year but has a relatively small impact on our day-to-day lives, but COVID has had a tremendous impact on people all over the world. So should COVID be downplayed?
Local health care workers say no, particularly because medical professionals are constantly learning new things about COVID-19.
Doctors already know a great deal about seasonal influenza. Strains of influenza are detected year-round in the United States, and have been for a long time, according to the Centers for Disease Control and Prevention. Flu viruses are most common in the fall and winter. Influenza activity typically begins to increase in October and peaks between December and February, but it can last as late as May.
COVID-19, on the other hand, only recently exposed itself to the world. The first United States cases of nontravel–related COVID-19 were confirmed in late February. Although coronaviruses are common — human coronaviruses were first identified in the mid-1960s — the CDC says the COVID-19 strain hasn’t been seen in humans before, and it’s not the same as other coronaviruses that cause mild illness.
Flu and COVID-19 facts at a glance
When talking about the flu and COVID-19, it’s important to know the facts surrounding both of them. The following lists contain information EastIdahoNews.com gathered from the CDC, as well as state and local healthcare providers.
Flu facts
What type of virus is the flu?: A respiratory illness caused by various strains of the influenza virus.
Who is at risk for contracting the flu?: Anybody can get the flu. Serious problems related to the flu can happen at any age, but some people are at high risk of developing serious flu-related complications such as those 65 years and older, people with certain chronic medical conditions, pregnant women and children younger than 5 years old.
Symptoms of the flu: Fever or feeling feverish/chills, cough, sore throat, runny or stuffy nose, muscle or body aches, headaches, and fatigue. Some people may have vomiting and diarrhea.

How long do symptoms appear after exposure?: From the time a person is exposed and infected with the flu to when symptoms begin is about two days, but it can range from about one to four days.
How long does the flu last?: Most people who get the flu will recover in a few days to less than two weeks. Sometimes people develop complications as a result of the flu, which can result in death.
How does the flu spread?: Most experts believe flu viruses spread mainly by tiny droplets produced when people cough, sneeze or talk. Sometimes, though not as often, a person might get the flu by touching a surface or object that has the flu virus on it and then touching their mouth, nose or possibly their eyes.
Flu recovery: Doctors may prescribe antivirals for treating the flu. It’s recommended those with the flu avoid contact with other people. If a person must leave home, they should wear a mask or cover coughs and sneezes with a tissue, and wash their hands often.
COVID-19 facts
What type of virus is COVID-19?: A respiratory illness caused by infection with a new coronavirus called SARS-CoV-2.
Who is at risk for contracting COVID-19?: Anybody can get COVID-19. Older adults and people who have severe underlying medical conditions seem to be at higher risk for developing more serious complications.
Symptoms of COVID-19: The virus is new, and we’re still learning about it. Some of the possible COVID-19 symptoms include fever or chills, cough, shortness of breath or difficulty breathing, fatigue, muscle or body aches, headache, loss of taste or smell, sore throat, congestion or runny nose, nausea, or vomiting and diarrhea.
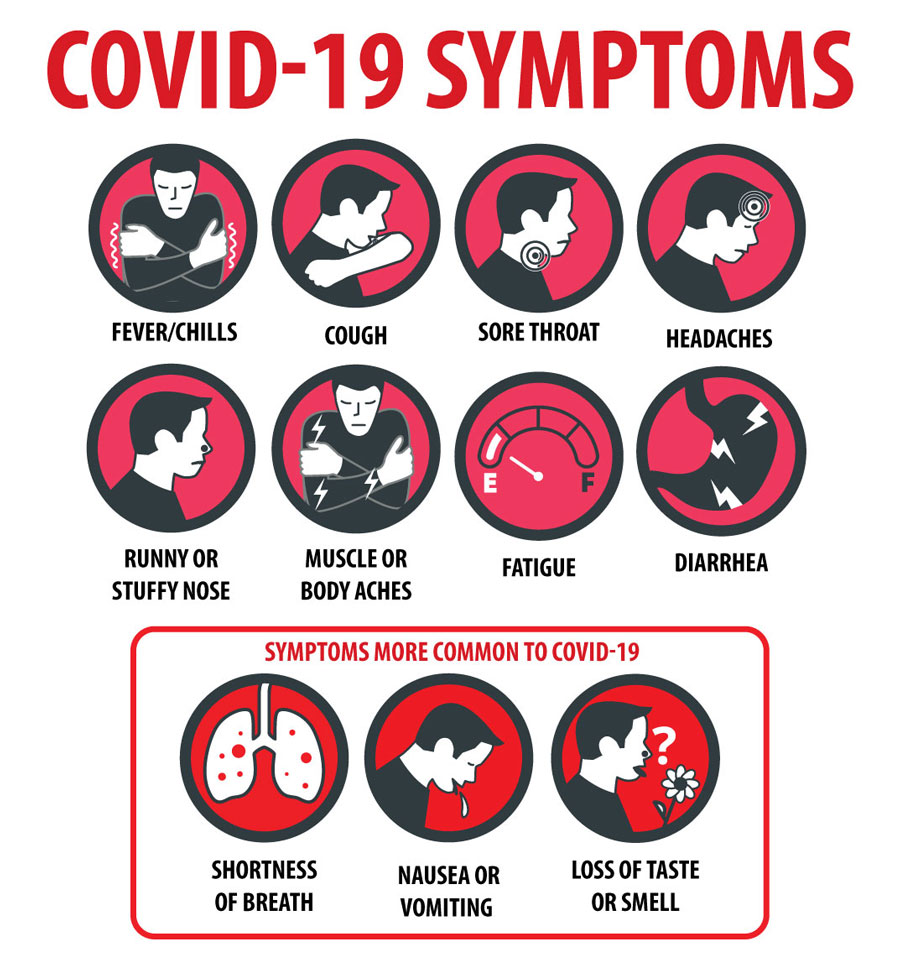
How long do symptoms appear after exposure?: Symptoms may appear two to 14 days after being exposed to COVID-19.
How long does COVID-19 last?: For most people who get COVID-19, isolation and precautions can generally be discontinued 10 days after symptoms first appear and after at least 24 hours have passed with no fever (without the use of fever-reducing medications) and with the improvement of other COVID-19 symptoms.
How does COVID-19 spread?: It’s thought that COVID-19 spreads mostly from person to person, mainly through respiratory droplets made when an infected person coughs, sneezes or talks.
COVID-19 recovery: If a person contracts COVID-19, it’s recommended they isolate themselves. If the person must be around people or animals in or outside of their home, they should wear a mask.
RELATED | FACT OR FICTION: Local medical and legal experts weigh in on masks
Can the flu and COVID-19 really be compared to each other?
The CDC estimates that in the U.S., influenza has resulted in between 9 million to 45 million illnesses, between 140,000 to 810,000 hospitalizations, and between 12,000 to 61,000 deaths annually since 2010. There has been an estimated 359,000 flu deaths in total during the last decade. The low point (12,000) was during the 2011-2012 season. The high point (61,000) was in the 2017-2018 season.
According to a 2019-2020 Influenza Season Surveillance Summary, the Idaho Department of Health and Welfare reported the number of influenza-related deaths that occurred from Oct. 5, 2019, through May 2, 2020, in Idaho was 39.
When looking at COVID-19 statistics in the U.S., the CDC COVID Data Tracker shows more than 7 million total cases, more than 210,000 deaths and almost 60,000 hospitalizations.
Idaho has had more than 45,000 COVID-19 cases (confirmed and probable) and more than 500 deaths as of Monday.
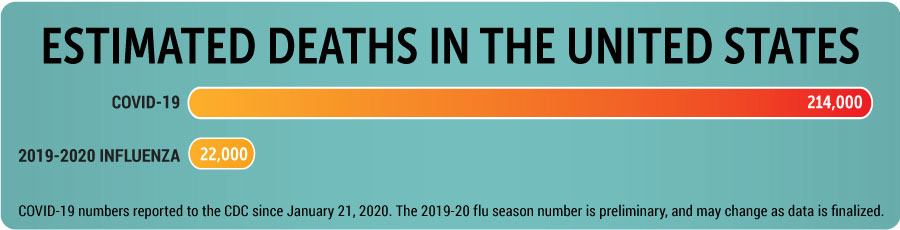
But skimming over the flu and COVID-19 statistics doesn’t give the most accurate picture. Unlike COVID-19, the flu is not a reportable disease in Idaho, so it is not tracked, but influenza-related deaths are reported by the Idaho Bureau of Vital Records and Health Statistics during influenza season.
“I don’t know why flu is left off that (reportable disease list) and why it wouldn’t be included, other than it’s a very common one throughout and it’s reoccurring every year,” Eastern Idaho Public Health Community Health Division Director James Corbett said.
Corbett said the flu already has some protective measures in place, such as a vaccine and herd immunity, whereas when COVID hit, everybody was 100% susceptible to catching it.
“With (COVID-19) being a novel (new) virus, we really only have (had) seven months (with it),” he said. “So far, it has not been a seasonal-type virus, which flu is. It’s really hard to compare a seasonal type virus with a nonseasonal virus.”
He said EIPH still tries to capture how much flu is circulating so that if there is a problem, the health district can be aware of it and help educate people, but he added there are steps that can be taken now so people can protect themselves from the viruses.
“Those same general mitigation strategies (for COVID-19) work for flu as well, except for with the added benefit of having a flu vaccine each year,” Corbett said.
Local doctors answer five popular flu, COVID-19 questions
EastIdahoNews.com spoke with Eastern Idaho Regional Medical Center Infectious Disease Medical Director John Bagwell and Idaho Falls Community Hospital Chief of Internal Medicine Dr. Scott Taylor to get answers to some of the most frequently asked flu versus COVID-19 questions. Their answers have been edited for length.
EastIdahoNews.com: As we approach flu season with COVID-19 still present, which one should people be more concerned about?
Bagwell: I think it’s turned out to be COVID is going to be the one that people should be more concerned about. I mean, flu is definitely a problem for some patients, but it’s not the overall worry that COVID-19 is.
But both of them are very serious too, in the right patient population. Influenza seems to affect the very young, more so than COVID, so that’s a concern. Influenza affects the very elderly, also similar to coronavirus.
Taylor: I think that is a complex question. For the general population, taking both equally serious is important. However, the risk of life-threatening consequences with COVID-19, especially for the elderly and patients with comorbid (simultaneous) conditions, create significant concerns in these populations for a worse outcome with COVID-19.
EastIdahoNews.com: How might COVID-19 affect this year’s flu season?
Bagwell: I’m an optimist here. I’m basing this based upon what happened in the southern hemisphere, in Australia in particular. Their season is the opposite of ours, so they’re finishing up their flu season. They remarkably had about 21,000 cases all flu season compared to (about) 250,000, the year before. It’s very possible that we might have a milder flu season, and mainly because of the mitigation strategies with masking that we’re doing. They (also) had a lot more people get flu shots than they normally had.
I think the combination of a vaccination effort and the masking made a big difference to the flu season. I’m hopeful that’s going to translate to the U.S., but you never know.
Taylor: There’s been different thoughts about this. One thought is that the flu season might actually be much improved because people are taking precautions to protect themselves from COVID-19. There’s also the hope the coronavirus outbreak will incentivize more people to get their flu vaccinations, giving more protective coverage for our communities from influenza.
I think it’ll be a pretty standard flu season, personally. But there is a theory that it might actually be better. There’s also the concern that on a rare occurrence, somebody could get both influenza and COVID-19. That dual pathogen effect might make people more severely ill, although I think that’ll be a pretty rare thing.
EastIdahoNews.com: What is the biggest difference between the flu and COVID-19?
Bagwell: Most of the time, the flu and COVID are going to be very similar. You’re going to have a fever, myalgias (muscle pain), feel bad, have a cough and a sore throat. The respiratory components are very similar, but COVID causes a lot of other different problems that you don’t see with flu.
COVID causes your blood to clot. That causes all kinds of problems. A lot of the morbidity and mortality we’re seeing with COVID comes from this tendency to form blood clots everywhere.
It’s going to be hard to tell the two apart. You’re going to have to have tests. Fortunately, we do have very good tests available to differentiate the two that are very accurate.
Taylor: I think there are several notable differences, the most notable being the way you can protect yourself. Influenza, we have a functional vaccine that you can protect yourself before even catching that. Also with influenza, we have treatment plans that are both proven and reasonably priced.
The third thing that differs them is even though you can become severely ill with either one, there is a tendency for people with more comorbidities — including age, obesity, immunosuppression and multiple other illnesses — to get more life-threatening illness with the COVID virus than influenza.
Younger patients (also) tend to get probably sicker with influenza and not as sick with COVID.
EastIdahoNews.com: Why do people make the comparison that the flu and COVID-19 are the same?
Bagwell: I think they do that because like what I said, the respiratory component to both illnesses are very similar with the high fever, achiness, don’t feel good with a cough. If you get short of breath, it’s probably more likely to be COVID than it would be influenza.
But again, a lot of people with COVID don’t ever get short of breath, so it’s difficult to tell sometimes. Some people get sniffles, a runny nose and a sore throat with COVID, and the same thing happens with influenza.
Taylor: I think because they’re both respiratory pathogens. They have very similar symptomatology in general (such as) fevers, body aches, headaches, and then pulmonary symptoms (such as) cough, shortness of breath and the possibility of a pneumonia-like picture in either one. They both are spread similarly in respiratory secretions.
EastIdahoNews.com: What complications can result from COVID-19? What complications can result from the flu?
Bagwell: Getting back to what I was saying earlier, the tendency to form blood clots is a big problem with COVID. It causes all kinds of complications, and it can include heart attacks (and) pulmonary embolism, which is a blood clot in the lungs. All of those could be lethal.
The other thing that could happen that we see not infrequently is strokes, and they’re caused by blood clots that are directly related to COVID.
Most people (with the flu) recover without any sequelae (aftereffects) at all, except maybe some fatigue that persists for a month or so, but that’s usually it.
Taylor: COVID is still so new to the medical community (that) long term, if there are any complications, (it’s) really hard to say. Right now, you would say that people still have complications of shortness of breath, fatigue — being tired for 10 to 12 weeks after getting COVID — that’s what we’ve seen the most of. We’ve seen some people have chronic shortness of breath.
There have been other things in the media (such as) cardiac abnormalities, which can happen with both influenza and COVID where it affects the heart muscle, or has some long-term effect, but those are pretty rare.
The biggest things are going to be once you get over the illness, getting through your body being worn down, getting your strength and muscle mass back and getting your nutritional status back to normal.
Prevention tips
The Idaho Department of Health and Welfare reminds people during the pandemic to keep at least 6 feet between you and others in public, wear face coverings in public places, stay home if you are sick, wash your hands often, cover coughs and sneezes and disinfect surfaces and objects regularly.
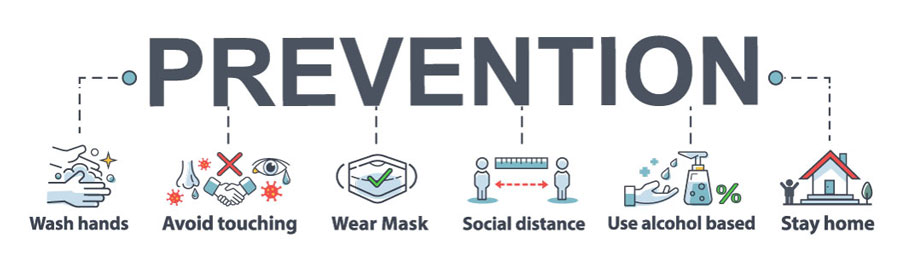
Bagwell and Taylor said along with those recommendations, you can take action now to help fight flu season during COVID-19.
“We’re really making a huge push to try to increase flu vaccination efforts to get more people vaccinated,” Bagwell explained. “I’m hopeful if we do the same thing in the U.S. (that Australia did), we can get the same kind of results.”
For more COVID-19 news and local statistics, click here.



